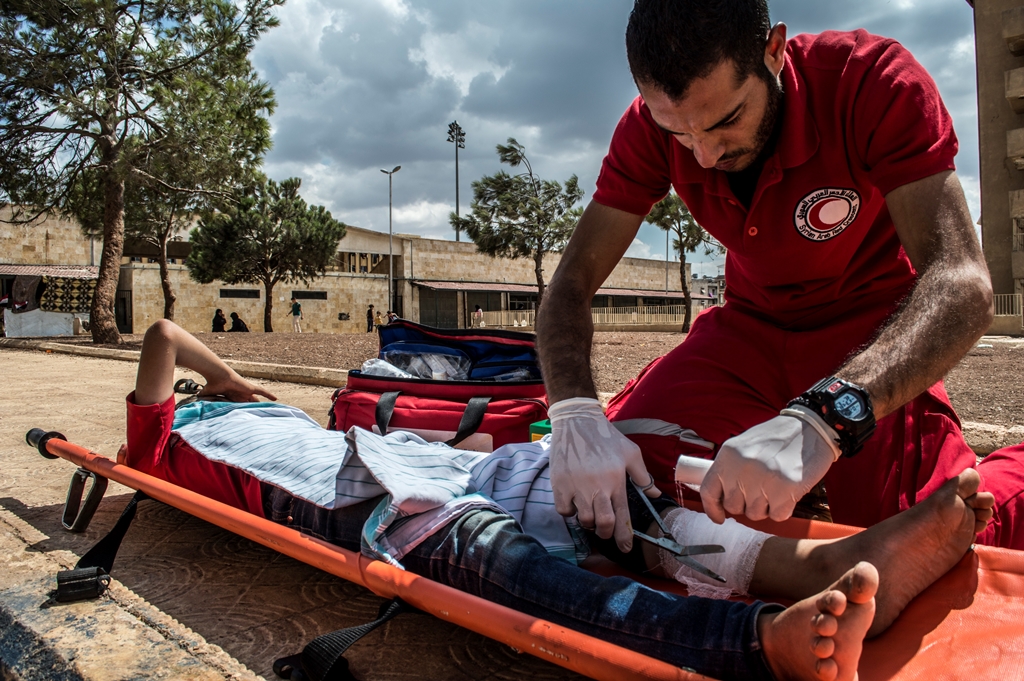
Public Health
Disasters change the landscape in numerous ways and only a portion of the changes are immediately evident. This is especially true when it comes to public health, which encompasses efforts to protect and improve the health of communities as a whole.
Overview
Disasters change the landscape in numerous ways and only a portion of the changes are immediately evident. This is especially true when it comes to public health, which encompasses efforts to protect and improve the health of communities as a whole. This includes the promotion of healthy lifestyles, research into the prevention of injury, disease and education. The healthier the community, and the more resources it has before disaster strikes, the greater resilience that community will show.
The impact a disaster has on an affected population’s health is far from predictable. A variety of factors influence the spread of disease and other health-related issues following an event. And, many can be mitigated with thoughtful pre-planning since one of the key factors related to disease spread and health after a disaster is connected to access. This is dependent upon the amount of destruction the disaster causes and the displacement of medical professionals and evacuees. Disaster preparedness efforts that consider, for example, health facility capabilities, reproductive health, mental health and water, sanitation and hygiene greatly lessen the toll of sickness on impacted populations.
A prime example of a catastrophic failure in public health occurred in Puerto Rico in the wake of 2017’s Hurricane Maria. The official death toll from the Category 4 hurricane stood at 64 for months after the storm because the disaster strained resources to the point where the dead were not counted or the government was uncertain how to determine what constituted a disaster-related death. In August 2018, the death toll was raised to 2,975 after more thorough research through an independent study. Puerto Rico was already struggling to maintain its public health before Maria significantly damaged key infrastructure across the island. Not only did hospitals receive direct damage in the storm, some were unable to access electricity or fuel for generators for significant amounts of time.
Key Facts
- Disaster-related health needs typically do not show up immediately. Some health concerns will not appear until much later, especially in terms of mental health. Consider the challenges of survival after livelihoods have been lost, such as the loss of livestock representing years of accumulated family wealth or ongoing issues following the death of the head of a household.
- Damage to health care facilities—and diagnostic equipment—can have long-reaching consequences. So, too, can damage to infrastructure such as roads and bridges that prevents people from being able to connect to services they need. In addition, losses that affect the personal lives of healthcare workers also affect the ability of health facilities to provide services.
- Water, sanitation and hygiene conditions before and after a disaster can greatly affect the level of impact on a community’s health. Drinking water supply and waste management are especially important factors in controlling disease, as is the management of toxic substances released by the disaster.
- Often, post-disaster outbreaks of disease are associated with population displacement. Widespread disasters such as hurricanes, famine or floods can result in large groups of people being evacuated to crowded facilities. Since disease tends to spread in overcrowded areas, without proper access to health care services, the evacuation conditions themselves can contribute to disease transmission. In resource-poor areas, already decreased nutritional status and lack of vaccinations can also contribute to the problem. Sometimes this can mean outbreaks of diarrhea, but other times, it could be respiratory infections or conjunctivitis with so many people in close quarters.
- Some health crises do not follow a natural disaster — they are disasters in their own right. Pandemics like the 2018 Ebola outbreak in the Democratic Republic of the Congo – and other disease outbreaks create public health concerns that act as a disaster by creating a community crisis, as well as a public health crisis Healthcare workers constituted five percent of the infected, in many cases due to the need to treat people without wearing protective equipment.
- Disasters can exacerbate reproductive health needs. Along with damage to facilities, equipment, medications and other infrastructure, access to services could be decreased. Frequently, other concerns can take higher priority. In addition, periods of high stress, overcrowding in temporary relief situations and hygiene-related challenges could increase the chance of sexually-transmitted diseases and gender-based violence.
- There is no health without mental health. The Center for Disaster Philanthropy has prepared an issue insight on Mental Health and Trauma needs during and after a disaster.
How to Help
Opportunities for reducing the health impact of disasters abound. Interested donors could:
- Support local efforts to bolster critical services and build community resilience. On a larger scale, strengthen water treatment and sewer facilities to better withstand disasters. On a smaller, but equally important, scale, fund efforts to improve health care equipment, support hygiene programs and ensure plans for mental health access are in place.
- Fund efforts to ensure post-disaster reproductive care and access. Consider both immediate needs and long-term concerns, including birth control, pregnancy, sexually-transmitted diseases and efforts to reduce gender-based violence in overcrowded displaced populations.
- Fund risk reduction activities such as vulnerability assessments for potentially disaster-prone areas and impact mitigation. Fund the creation of rapid needs assessments to collect reliable data about the needs of affected communities after disasters occur. In addition, identify marginalized and vulnerable populations that suffer the most in disasters and assess their unique needs. In terms of mitigating impact, include the creation of public health communications that are reliable, accessible, consistent and culturally relevant.
- Fund training for healthcare providers to identify and strengthen the most vulnerable populations. Recognize that different populations may be more vulnerable to different disasters.
- Support programs that assist caregivers in disaster-affected areas. They may be coping with their own grief while assisting others.
- Fund the transfer of paper files to electronic medical records. These are less likely to be destroyed during a disaster or lost or misplaced following a disaster.
- Support research into the ongoing effects of disasters on populations, as well as effective ways to build coping capacities among individuals and communities. This research should focus on the differential impacts on vulnerable populations.
What Funders Are Doing
- Kaiser Permanente Corporate Giving Program gave $1 million in 2017 to the Centers for Disease Control (CDC) to support public health in Puerto Rico following Hurricane Maria.
- In 2016, the Coca-Cola Foundation gave $500,000 to Uniting for Health Innovation to help mitigate the ongoing cholera outbreak in Haiti stemming from the 2010 earthquake.
- The New Venture Fund gave $100,000 in 2017 to Public Health Institute to promote public safety and disaster preparedness.
- The Robert Wood Johnson Foundation gave $150,000 in 2017 to the National Academy of Sciences to provide support to the Forum on Medical and Public Health Preparedness for Disasters and Emergencies.
Learn More
- Pan American Health Organization: Natural Disasters: Protecting the Public’s Health
- Centers for Disease Control and Prevention: Epidemics after Natural Disasters
- National Academy of Science: Linking Hazards and Public Health: Case Studies in Disasters
- World Health Organization: Communicable Diseases Following Natural Disasters
We welcome republication of our content. Please credit the Center for Disaster Philanthropy.